What mobitz 1
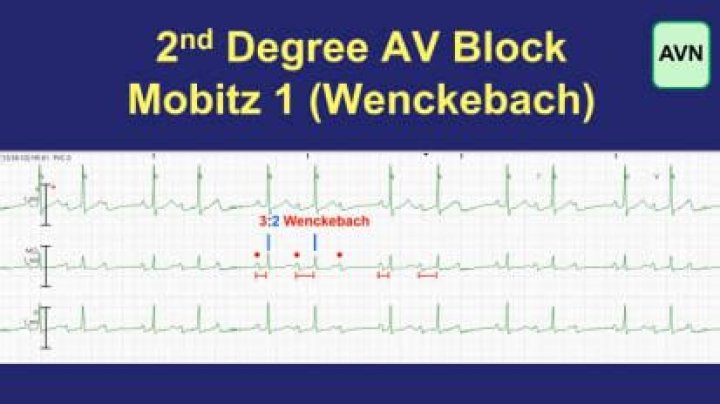
Mobitz type 1 block is characterized by a gradual prolongation of the PR interval
Does mobitz type 1 need treatment?
In the emergency room type 1 Mobitz block without symptoms requires no treatment. However, symptomatic patients may be managed with atropine or transvenous pacing and a cardiology consult should be obtained. The patient must be admitted to a monitored unit.
Is mobitz type 1 benign?
Traditionally Wenckebach second degree atrioventricular (AV) block (Mobitz I) has been considered benign.
What is the difference between mobitz I and mobitz II?
Unlike Mobitz I, which is produced by progressive fatigue of the AV nodal cells, Mobitz II is an “all or nothing” phenomenon whereby the His-Purkinje cells suddenly and unexpectedly fail to conduct a supraventricular impulse.What is mobitz Type 1 second degree AV block?
Also called Wenckebach or Mobitz type I block, type I second-degree AV block occurs when each successive impulse from the SA node is delayed slightly longer than the previous one. This pattern of progressive prolongation of the PR interval continues until an impulse fails to be conducted to the ventricles.
Is mobitz Type 1 sinus rhythm?
Mobitz type I is a type of 2nd degree AV block, which refers to an irregular cardiac rhythm (arrhythmia), that reflects a conduction block in the electrical conduction system of the heart.
What does mobitz 1 look like?
Mobitz type 1 block is characterized by a gradual prolongation of the PR interval over a few heart cycles until an atrial impulse is completely blocked, which manifests on the ECG as a P-wave not followed by a QRS complex. This cycle repeats itself over and over again, such that every cycle ends with a blocked P-wave.
What is the heart block?
Heart block is a condition where the heart beats more slowly or with an abnormal rhythm. It’s caused by a problem with the electrical pulses that control how your heart beats.How common is mobitz 1?
How common are heart blocks? First degree and Mobitz type 1 heart blocks are uncommon but not rare. It is estimated that 0.5-2% of otherwise healthy adults have these types of heart blocks.
Is first-degree heart block serious?First-degree heart block is the least severe. The electrical signals slow down as they move from your atria to your ventricles. First-degree heart block might not require treatment of any kind. Mobitz type I: The electrical signals get slower and slower between beats.
Article first time published onIs second-degree heart block serious?
Second-degree heart block may develop into a more serious type of heart block. It may cause a sudden loss of consciousness or it may cause the heart to suddenly stop beating.
What causes first-degree heart block?
First-degree heart block may be caused by: Natural aging process. Damage to the heart from surgery. Damage to the heart muscle from a heart attack.
What causes 2nd degree type 1 Heartblock?
There are multiple causes of second-degree Mobitz type 1 (Wenckebach) AV block, including reversible ischemia, myocarditis, increased vagal tone, status post-cardiac surgery, or even medications that slow AV nodal conduction (e.g., beta-blockers, non-dihydropyridine calcium channel blocks, adenosine, digitalis, and …
Is there ap wave for every QRS complex?
In blocks with 2:1 conduction, two P waves occur for every QRS complex, indicating every other impulse is blocked, as shown in the strip below.
What is mobitz II?
Type 2 Second-degree AV block, also known as Mobitz II, is almost always a disease of the distal conduction system (His-Purkinje System). Mobitz II heart block is characterized on a surface ECG by intermittently non conducted P waves not preceded by PR prolongation and not followed by PR shortening.
What is a pacemaker spike?
It shows pacemaker spikes: vertical signals that represent the electrical activity of the pacemaker. Usually these spikes are more visible in unipolar than in bipolar pacing. In the first example, the atria are being paced, but not the ventricles, resulting in an atrial paced rhythm.
What medications cause heart block?
Common drugs that induce atrioventricular (AV) block include beta-blockers, calcium channel blockers, antiarrhythmics, and digoxin. Withdrawal of the offending drugs is the first treatment for heart block.
Can you live with heart blockage?
According to the Centers for Disease Control and Prevention (CDC), around one-half of all people diagnosed with congestive heart failure will survive beyond five years.
What is 1st and 2nd degree heart block?
First-degree heart block: The electrical impulse still reaches the ventricles, but moves more slowly than normal through the AV node. The impulses are delayed. This is the mildest type of heart block. Second-degree heart block is classified into two categories: Type I and Type II.
What is a 3 1 heart block?
3:1 block. The atrial rate (purple arrows) is approximately 90 bpm. The ventricular rate rate is approximately 30 bpm. Note how every third P wave is almost entirely concealed within the T wave.
What is 3rd degree block?
Third-degree atrioventricular (AV) block, also referred to as third-degree heart block or complete heart block (CHB), is an abnormal heart rhythm resulting from a defect in the cardiac conduction system in which there is no conduction through the atrioventricular node (AVN), leading to complete dissociation of the …
What's the lowest your heart can beat?
Normally, your heart beats 60 to 100 times a minute when you’re at rest. But with bradycardia, it goes down to less than 60 beats a minute.
Can heart block cure itself?
Heart block occurs when the electrical signal is slowed down or does not reach the bottom chambers of the heart. Your heart may beat slowly, or it may skip beats. Heart block may resolve on its own, or it may be permanent and require treatment.
What is a flutter in the heart?
Atrial flutter is a type of abnormal heart rhythm, or arrhythmia. It occurs when a short circuit in the heart causes the upper chambers (atria) to pump very rapidly.
What is the treatment for 1st degree AV block?
In general, no treatment is required for first-degree AV block unless prolongation of the PR interval is extreme (>400 ms) or rapidly evolving, in which case pacing is indicated. Prophylactic antiarrhythmic drug therapy is best avoided in patients with marked first-degree AV block.
What is the treatment for heart block?
There is no heart-block-specific treatment. Most people with bundle branch block have no symptoms, and they do not require treatment. However, any underlying causes, such as hypertension, will need treatment. Share on Pinterest Patients with second- or third-degree heart block may need a pacemaker.
Can AV block cause death?
Patients with third-degree atrioventricular (AV) block (complete heart block) are frequently hemodynamically unstable; as a result, they may experience syncope, hypotension, cardiovascular collapse, or death.
What heart block feels like?
Typical symptoms of heart block are similar to those of many other arrhythmias and may include dizziness, lightheadedness, fainting, fatigue, chest pain, or shortness of breath. Some patients, especially those with first-degree heart block, may not experience symptoms at all.
How do you get rid of a blocked heart without surgery?
Through angioplasty, our cardiologists are able to treat patients with blocked or clogged coronary arteries quickly without surgery. During the procedure, a cardiologist threads a balloon-tipped catheter to the site of the narrowed or blocked artery and then inflates the balloon to open the vessel.
Is 1st degree AV block normal?
In general, a first-degree AV block is a benign finding that does not require any treatment. However, it may be an indicator of higher-degree AV block in the future and, depending on the PR interval, AV blocking medications may be avoided.
Can heart block be treated with medicine?
Medication as effective as stents, bypass for treating blocked arteries, major study shows. The findings of the ISCHEMIA trial could be a game-changer for cardiology, and for patients with stable coronary artery disease.