What is the meaning of CLD
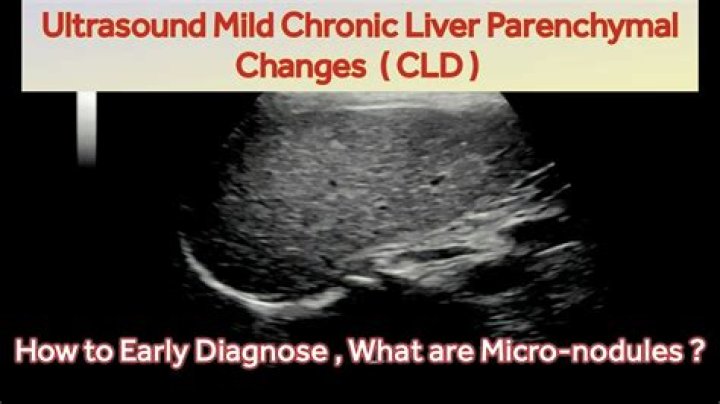
Chronic Liver Disease (CLD) Treatment.
What CLD means?
Definition of chronic liver disease (CLD) Progressive destruction of the liver parenchyma over a period greater than 6 months leading to fibrosis and cirrhosis.
What is the treatment of CLD?
Cirrhosis CLD Treatment Stop drinking alcohol. Limit salt in the diet. Eat a nutritious diet. Get vaccinated for influenza, hepatitis A and hepatitis B, and pneumococcal pneumonia (if recommended by your doctor).
What is cause of CLD?
The most common causes are hepatitis and other viruses, and alcohol abuse. Other medical problems can also cause it. The damage to the liver usually can’t be reversed.What is Cryptogenic CLD?
Collapse Section. Cryptogenic cirrhosis is a condition that impairs liver function. People with this condition develop irreversible liver disease caused by scarring of the liver (cirrhosis), typically in mid- to late adulthood.
Is chronic liver disease serious?
Even more severe symptoms can develop if the liver disease is extreme; the liver can be severely damaged and stop working, resulting in a number of toxins in the blood. Sufferers can even die from complications from chronic liver disease such as liver cancer.
Does fiber help your liver?
Eat food with fiber: Fiber helps your liver work at an optimal level. Fruits, vegetables, whole grain breads, rice and cereals can take care of your body’s fiber needs. Drink lots of water: It prevents dehydration and it helps your liver to function better.
How do you test for CLD?
- Liver function tests: blood tests can help look for genetic conditions or viral hepatitis.
- CT scan, MRI, or ultrasound: imaging tests can look for sequelae of chronic liver damage.
- Liver biopsy: a long needle is inserted into the skin to remove a tissue sample of the liver for further study.
What are the 4 stages of liver disease?
- Causes of Liver Disease. Liver disease refers to any condition that negatively impacts your liver. …
- Stages of Liver Disease. …
- Stage 1: Inflammation. …
- Stage 2: Fibrosis. …
- Stage 3: Cirrhosis. …
- Stage 4: Liver Failure.
Cirrhosis isn’t curable, but it’s treatable. Doctors have two main goals in treating this disease: Stop the damage to your liver, and prevent complications. Alcohol abuse, hepatitis, and fatty liver disease are some of the main causes.
Article first time published onWhat are signs that your liver is struggling?
- Fatigue and tiredness. …
- Nausea (feeling sick). …
- Pale stools. …
- Yellow skin or eyes (jaundice). …
- Spider naevi (small spider-shaped arteries that appear in clusters on the skin). …
- Bruising easily. …
- Reddened palms (palmar erythema). …
- Dark urine.
What are signs that your liver is not functioning properly?
- Skin and eyes that appear yellowish (jaundice)
- Abdominal pain and swelling.
- Swelling in the legs and ankles.
- Itchy skin.
- Dark urine color.
- Pale stool color.
- Chronic fatigue.
- Nausea or vomiting.
What are the signs of dying from cirrhosis of the liver?
- Loss of appetite.
- Weakness.
- Fatigue.
- Nausea/Vomiting.
- Abdominal pain/bloating.
- Itching.
What is other cirrhosis of the liver?
Cirrhosis is a late stage of scarring (fibrosis) of the liver caused by many forms of liver diseases and conditions, such as hepatitis and chronic alcoholism. Each time your liver is injured — whether by disease, excessive alcohol consumption or another cause — it tries to repair itself.
What does steatohepatitis mean?
A type of liver disease in which fat builds up in the liver of people who drink little or no alcohol. This causes inflammation of the liver and damage to the cells in the liver, which may lead to cirrhosis (scarring of the liver) and liver failure.
Which fruit is best for liver?
Fill your fruit basket with apples, grapes and citrus fruits like oranges and lemons, which are proven to be liver-friendly fruits. Consume grapes as it is, in the form of a grape juice or supplement your diet with grape seed extracts to increase antioxidant levels in your body and protect your liver from toxins.
Is lemon good for liver?
Lemons are rich in Vitamin C and protect liver from oxidative damage. You must drink lemon in warm water every morning to reap the best benefits or add it in Green Tea for a double dose of good health.
Which vegetables are good for liver?
Cruciferous vegetables like broccoli and Brussels sprouts may help increase the liver’s natural detoxification enzymes, protect it from damage, and improve blood levels of liver enzymes.
Can you live with chronic liver disease?
Cirrhosis has become irreversible. Diagnosed at stage 3, the 1-year survival rate is 80%. It’s during stage 3 that a liver transplant may be recommended. There’s always a risk a person’s body will reject the transplant, but if accepted, 80% of transplant patients survive more than 5 years past their operation.
What stage is chronic liver disease?
Chronic liver failure, also called end-stage liver disease, progresses over months, years, or decades. Most often, chronic liver failure is the result of cirrhosis, a condition in which scar tissue replaces healthy liver tissue until the liver cannot function adequately.
How long can you live with chronic liver disease?
Patients with compensated chronic liver failure (without ascites, variceal bleeding, encephalopathy, or jaundice) have a median survival of 12 years. After decompensation, median survival drops to ~ 2 years.
Can liver damage be repaired?
The liver is a unique organ. It is the only organ in the body that is able to regenerate. With most organs, such as the heart, the damaged tissue is replaced with scar, like on the skin. The liver, however, is able to replace damaged tissue with new cells.
Can you live without a liver?
The liver performs essential, life-sustaining functions. While you can’t live without a liver completely, you can live with only part of one. Many people can function well with just under half of their liver. Your liver can also grow back to full size within a matter of months.
What happens when your liver fails?
Acute liver failure often causes complications, including: Excessive fluid in the brain (cerebral edema). Too much fluid causes pressure to build up in your brain, which can lead to disorientation, severe mental confusion and seizures. Bleeding and bleeding disorders.
Can endoscopy detect liver problems?
Liver disease and cirrhosis are common causes of mortality worldwide[1]. The role of endoscopy in liver disease is both diagnostic and interventional: endoscopy should be offered to patients with relevant symptoms (unsuspected liver disease may be diagnosed in this manner) and for variceal screening and treatment.
Where do you feel liver pain?
Most people feel it as a dull, throbbing sensation in the upper right abdomen. Liver pain can also feel like a stabbing sensation that takes your breath away. Sometimes this pain is accompanied by swelling, and occasionally people feel radiating liver pain in their back or in their right shoulder blade.
How do I make my liver healthy again?
- Maintain a healthy weight. …
- Eat a balanced diet. …
- Exercise regularly. …
- Avoid toxins. …
- Use alcohol responsibly. …
- Avoid the use of illicit drugs. …
- Avoid contaminated needles. …
- Get medical care if you’re exposed to blood.
What foods can damage your liver?
Too much refined sugar and high-fructose corn syrup causes a fatty buildup that can lead to liver disease. Some studies show that sugar can be as damaging to the liver as alcohol, even if you’re not overweight. It’s one more reason to limit foods with added sugars, such as soda, pastries, and candy.
How long can a person live with liver cirrhosis?
Life expectancy by stage Compensated cirrhosis: People with compensated cirrhosis do not show symptoms, while life expectancy is around 9–12 years. A person can remain asymptomatic for years, although 5–7% of those with the condition will develop symptoms every year.
Can you recover from cirrhosis of the liver?
There is no cure for cirrhosis, but removing the cause can slow the disease. If the damage is not too severe, the liver can heal itself over time.
What are the signs of last days of life?
- Breathing difficulties. Patients may go long periods without breathing, followed by quick breaths. …
- Drop in body temperature and blood pressure. …
- Less desire for food or drink. …
- Changes in sleeping patterns. …
- Confusion or withdraw.