What does aberrant conduction mean
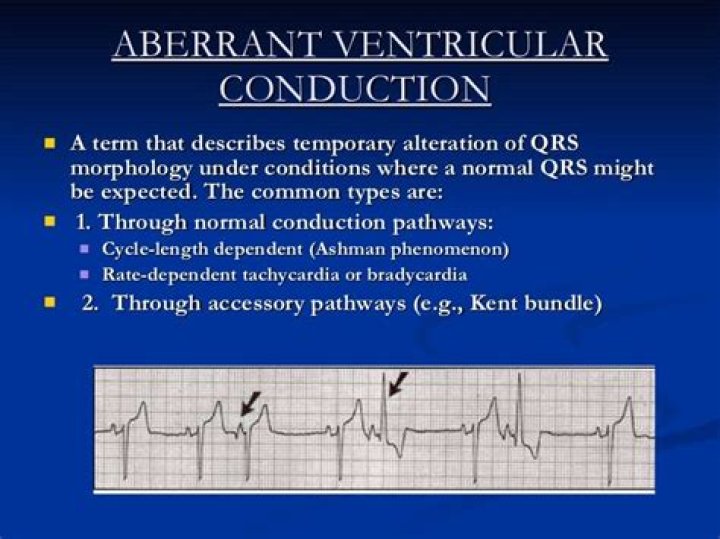
Aberrant conduction occurs when the length of the cardiac cycle is changed without a compensatory change in the length of the refractory period. This is explained by the changes of the refractoriness in the His-Purkinje system related to changes in the RR interval.
What does aberrant conduction mean in an ECG?
Aberrant ventricular conduction is a common electrocardiographic (EKG) manifestation that occurs when the supraventricular electrical impulse is conducted abnormally through the ventricular conducting system. This results in a wide QRS complex that may be confused with a ventricular ectopic beat.
How is aberrant conduction treated?
It is usually treated with vagal maneuvers or adenosine. What does aberrancy mean? You can think of “aberrancy” as abnormal conduction. When something is aberrant it “departs from the right, normal, or usual course.”
What is SVT with aberrant conduction?
Any tachycardic rhythm with a left or right bundle branch block that is NOT ventricular tachycardia is considered “supraventricular tachycardia with aberrancy”.Why do aberrant PACS occur?
Aberrant conduction occurs simply because the right and left bundle branches have different lengths of refractory periods. In Figure 2, the shaded area is the refractory period of the left and right bundle branches. As can be seen, one bundle branch, usually the right, has a longer refractory period than the other.
Is Sinus Arrhythmia serious?
Keep in mind that for the majority of people, a sinus arrhythmia is neither dangerous nor problematic. Even if your doctor suspects you have this irregular heartbeat, he may not order the test to check for it. That’s because an EKG can be costly, and a sinus arrhythmia is considered a benign condition.
What are two examples of aberrant conduction?
1) Atrial fibrillation( AF): Figure 2; 2) Atrial tachycardia; 3) Premature Atrial Contractions. In this case aberration occurs when a short cycle follows a long one.
Is SVT life threatening?
Supraventricular tachycardia is generally not life-threatening unless you have heart damage or other heart problems. However, in extreme cases, an episode of SVT may cause unconsciousness or cardiac arrest.How can AFIB be treated with Aberrancy?
If SVT with aberrancy, treat with IV adenosine (vagal maneuvers). For irregular WCTs, if atrial fibrillation with aberrancy, consider expert consultation; control rate. If pre-excited atrial fibrillation (AFIB + WPWS), expert consultation is advised. Avoid AV nodal blocking agents, consider amiodarone.
What is worse SVT or VT?Because VTs occur in the large pumping chambers of the heart, they make the heart extremely inefficient and are more serious than SVTs. The symptoms of VTs are usually more severe, and have a much greater tendency to be fatal.
Article first time published onWhat do premature atrial contractions feel like?
Symptoms of PVCs include a fluttering or flip-flop feeling in the chest, pounding or jumping heart rate, skipped beats and palpitations, or an increased awareness of your heartbeat.
Do beta blockers prevent ventricular tachycardia?
Furthermore, beta-blockers have been advocated for use in patients with ventricular fibrillation (VF) and ventricular tachycardia (VT), in whom these agents appear to reduce the incidence of recurrent ventricular tachyarrhythmias 6, 7.
When should I worry about PVCs?
PVCs become more of a concern if they happen frequently. “If more than 10% to 15% of a person’s heartbeats in 24 hours are PVCs, that’s excessive,” Bentz said. The more PVCs occur, the more they can potentially cause a condition called cardiomyopathy (a weakened heart muscle).
What is a junctional tachycardia?
Junctional tachycardia is a form of supraventricular tachycardia, a type of racing pulse caused by a problem in the area between the upper and lower chambers of your heart. It’s known as the atrioventricular node, or AV node.
What is the term for two PVCs back to back?
Given that a PVC occurs before a regular heartbeat, there is a pause before the next regular heartbeat. PVCs can occur in isolation or in repeated patterns. Two consecutive PVCs are termed doublets while three consecutive PVCs are named triplets.
How do you tell VT from sbert with Aberrancy?
Monomorphic VT Although there is a broad complex tachycardia (HR > 100, QRS > 120), the appearance in V1 is more suggestive of SVT with aberrancy, given that the the complexes are not that broad (< 160 ms) and the right rabbit ear is taller than the left.
What is a flutter in the heart?
Atrial flutter is a type of abnormal heart rhythm, or arrhythmia. It occurs when a short circuit in the heart causes the upper chambers (atria) to pump very rapidly.
What is AV dissociation in ECG?
Atrioventricular dissociation is a cardiac conduction defect where the atria and ventricles beat independently of each other. It can occur due to various pathological conditions, and a detailed ECG review is required to confirm the source.
What is the most common cause of sinus arrhythmia?
Sinus tachycardia is usually temporary and largely caused by stress, fever, exercise, or other outside conditions. In most cases, sinus tachycardia resolves itself on its own, but if it doesn’t, it could be a sign of a heart disease.
How do you fix sinus arrhythmia?
Treatments for sinus tachycardia focus on lowering the heart rate to normal by treating the underlying cause, such as infection or low blood pressure. Doctors may also recommend lifestyle changes, medications, and medical procedures, such as catheter ablation.
How do you get rid of sinus arrhythmia?
- Eliminate potential triggers or stimulants in your diet such as caffeine, nicotine, and alcohol.
- Take medicine to slow the heart rate such as ivabradine, beta-blockers, or calcium channel blockers.
- Exercise to improve quality of life and to maintain a healthy heart.
Is atrial flutter a narrow complex tachycardia?
The differential diagnosis of an irregular, narrow-complex tachycardia includes atrial fibrillation, atrial flutter with variable atrio-ventricular (AV) block and multifocal atrial tachycardia.
What causes AFib RVR?
Rapid ventricular rate or response (RVR) AFib is caused by abnormal electrical impulses in the atria, which are the upper chambers of the heart. These chambers fibrillate, or quiver, rapidly. The result is a rapid and irregular pumping of blood through the heart.
What class is procainamide?
Procainamide is a medication used to manage and treat ventricular arrhythmias, supraventricular arrhythmias, atrial flutter/fibrillation, and Wolf-Parkinson-White syndrome. It is in the antiarrhythmic Agent Class 1A class of medications.
Can SVT be caused by anxiety?
Some of the classic symptoms of a panic attack — a racing heart coupled with feeling breathless and dizzy — overlap with a condition known as supraventricular tachycardia, or SVT.
At what heart rate should you go to the hospital?
If you’re sitting down and feeling calm, your heart shouldn’t beat more than about 100 times per minute. A heartbeat that’s faster than this, also called tachycardia, is a reason to come to the emergency department and get checked out. We often see patients whose hearts are beating 160 beats per minute or more.
What is the most common cause of SVT?
Most episodes of SVT are caused by faulty electrical connections in the heart. SVT also can be caused by certain medicines. Examples include very high levels of the heart medicine digoxin or the lung medicine theophylline. Some types of SVT may run in families, such as Wolff-Parkinson-White syndrome.
What are the 5 lethal cardiac rhythms?
You will learn about Premature Ventricular Contractions, Ventricular Tachycardia, Ventricular Fibrillation, Pulseless Electrical Activity, Agonal Rhythms, and Asystole. You will learn how to detect the warning signs of these rhythms, how to quickly interpret the rhythm, and to prioritize your nursing interventions.
What is the survival rate for ventricular tachycardia?
Procedure mortality is approximately 3%, with most deaths due to failure of the procedure to control frequent, life-threatening VT.
What does SVT look like on a strip?
Classic Paroxysmal SVT has a narrow QRS complex & has a very regular rhythm. Inverted P waves are sometimes seen after the QRS complex. These are called retrograde p waves. The heart fills during diastole, and diastole is normally 2/3 the cardiac cycle.
Can you exercise with premature atrial contractions?
How can I reduce my risk of premature atrial contractions? Some risk factors, like aging, can’t be changed. However, you can: Exercise.