What does a GCS of 10 mean
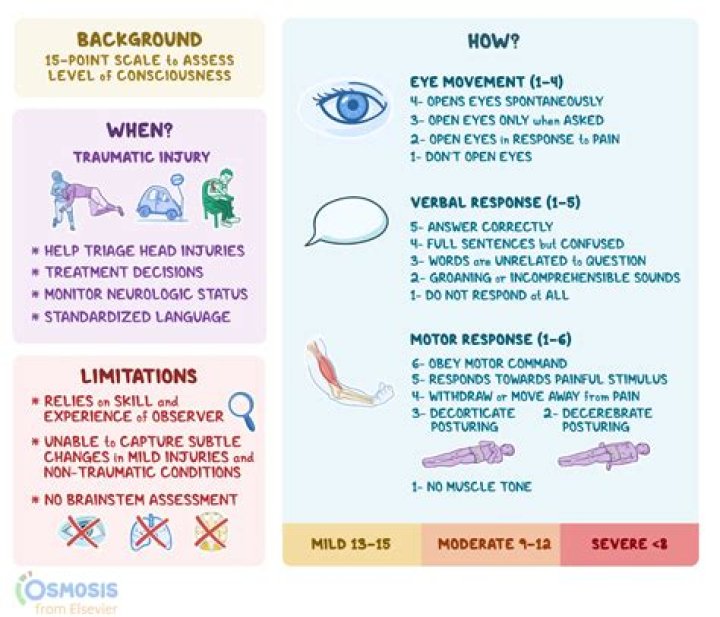
For example, a score of 10 might be expressed as GCS10 = E3V4M3. Best eye response (4) No eye opening. Eye opening to pain. Eye opening to sound.
Is GCS 10 bad?
Severe: GCS 8 or less. Moderate: GCS 9-12. Mild: GCS 13-15.
At what GCS do you intubate?
In trauma, a Glasgow Coma Scale score (GCS) of 8 or less indicates a need for endotracheal intubation. Some advocate a similar approach for other causes of decreased consciousness, however, the loss of airway reflexes and risk of aspiration cannot be reliably predicted using the GCS alone.
What is a good Glasgow Coma Scale score?
The components of the GCS should be recorded individually; for example, E2V3M4 results in a GCS score of 9. A score of 13 or higher correlates with mild brain injury, a score of 9 to 12 correlates with moderate injury, and a score of 8 or less represents severe brain injury.What will be the Glasgow Coma Scale score of a patient who has a moderate type of head injury?
It consists of 3 sections, each of which is scored: best motor response, best verbal response, and eye opening (Table 1). A total score of 3-8 for the 3 sections indicates severe TBI, a score of 9-12 indicates moderate TBI, and a score of 13-15 indicates mild TBI.
Is a high Glasgow Coma Scale good or bad?
Traumatic Brain Injury In the case of GCS scores of 3 to 5, mortality is high and success has generally been low, whereas for GCS scores of 6 to 8, aggressive triage and neurosurgical management may be the most important determinant of outcome.
What are the stages of a coma?
Three stages of coma DOC includes coma, the vegetative state (VS) and the minimally conscious state (MCS).
What is Glasgow Coma Scale 5?
Introduction: Patients presenting with an early Glasgow Coma Scale (GCS) Score of 3-5 after blunt or penetrating skull-brain assaults are categorized as having sustained a very severe traumatic brain injury (vs-TBI). This category is often overlooked in literature.How do you grade a Glasgow Coma Scale?
- Severe: GCS 3-8.
- Moderate: GCS 9-12.
- Mild: GCS 13-15.
Furthermore, the presence or absence of airway reflexes should not be assumed based on a patient’s GCS. The Glasgow coma scale can be utilized as one factor to help dictate airway management, but rigid use of a cut-off is not currently supported by robust evidence.
Article first time published onWhat is a GCS of 3t?
Threshold to consider intubation for airway protection (ATLS) = 8. Intubated patients are given a “t” for verbal, denoted as “GCS 3t”
What happens when a person is intubated?
To intubate, we basically put a breathing tube down the patient’s throat. Through that breathing tube, we attach them to a ventilator. This machine helps them exchange oxygen and carbon dioxide, supporting their breathing while they’re undergoing an operation or any kind of recovery.
What are the signs of Cushing's triad?
Cushing’s triad refers to a set of signs that are indicative of increased intracranial pressure (ICP), or increased pressure in the brain. Cushing’s triad consists of bradycardia (also known as a low heart rate), irregular respirations, and a widened pulse pressure.
Which Glasgow Coma Scale GCS data set indicates the most severe injury for a patient with traumatic brain injury and loss of consciousness?
The Glasgow Coma Scale (GCS) classifies Traumatic Brain Injuries (TBI) as Mild (14–15); Moderate (9–13) or Severe (3–8).
Can you pull the plug on someone in a vegetative state?
This means the patient would be unable to cough or swallow or breathe on her own, whereas a patient in a vegetative state may be able to do one or all of those three things, DiGeorgia said. … “Pulling the plug” would render the patient unable to breathe, and the heart would stop beating within minutes, he said.
How long can someone be on life support in a coma?
More invasive life support, such as heart/lung bypass, is only maintained for a few hours or days, but patients with artificial hearts have survived for as long as 512 days. Read more: Are near-death experiences just hallucinations? Do people in a coma dream?
How long does it take to come round from an induced coma?
Normally a patient in a medically induced coma would wake up over the course of a day. Some COVID patients are taking nearly a week to wake up.
What is an advantage of using Glasgow Coma Scale to assess level of consciousness?
Advantages of the Glasgow Coma Scale The most widely recognised of all conscious level scoring systems in the world. It has prognostic value: the motor score particularly has a significant impact on the prognosis. It is used to categorise traumatic brain injury into mild, moderate and severe.
What is the fastest way to calculate GCS?
To calculate the patient’s GCS , you need to add together the scores from eye opening, verbal response and motor response. Added together, these give you an overall score out of the maximum of 15.
How do you assess level of consciousness?
The tool we use to assess the level of consciousness is the Glasgow Coma Scale (GCS). This tool is used at the bedside in conjunction with other clinical observations and it allows us to have a baseline and ongoing measurement of the level of consciousness (LOC) for our patients.
What does GCS 15 mean in medical terms?
The GCS is the summation of scores for eye, verbal, and motor responses. The minimum score is a 3 which indicates deep coma or a brain-dead state. The maximum is 15 which indicates a fully awake patient (the original maximum was 14, but the score has since been modified).
Are all comatose patients intubated?
Conclusions: The majority of unconscious non-trauma patients were not intubated in the prehospital setting. Unconscious non-trauma patients may not all need tracheal intubation before being transferred to hospital.
What intubated means?
Intubation is a procedure that’s used when you can’t breathe on your own. Your doctor puts a tube down your throat and into your windpipe to make it easier to get air into and out of your lungs. A machine called a ventilator pumps in air with extra oxygen.
Why are patients intubated during surgery?
The primary purposes of intubation include: opening up the airway to give oxygen, anesthetic, or medicine. removing blockages. helping a person breathe if they have collapsed lungs, heart failure, or trauma.
What does a GCS of 9 mean?
Mild head injuries are generally defined as those associated with a GCS score of 13-15, and moderate head injuries are those associated with a GCS score of 9-12. A GCS score of 8 or less defines a severe head injury.
Why is it called the Glasgow Coma Scale?
The 1974 first version of a tool used to define severe head injury was known as the Coma Index. … In the famous 1974 Lancet article, Teasdale and Jennett introduced the Glasgow Coma Scale as a practical scale for assessing the depth and duration of impaired consciousness and coma.
How long can a person be on a ventilator in an ICU?
Some people may need to be on a ventilator for a few hours, while others may require one, two, or three weeks. If a person needs to be on a ventilator for a longer period of time, a tracheostomy may be required.
Is intubation the same as life support?
“Intubating a patient and putting them on a ventilator to help them breathe definitely means they are being put on life support, which is very scary to think about when it’s you or your loved one needing that treatment.”
Is intubation the same as ventilator?
Intubation is placing a tube in your throat to help move air in and out of your lungs. Mechanical ventilation is the use of a machine to move air in and out of your lungs.
What organs does Cushing's disease affect?
A noncancerous (benign) tumor of the pituitary gland, located at the base of the brain, produces an excess amount of ACTH , which in turn stimulates the adrenal glands to make more cortisol. When this form of the syndrome develops, it’s called Cushing disease.
What is Cushings response?
The Cushing reflex (vasopressor response, Cushing reaction, Cushing effect, and Cushing phenomenon) is a physiological nervous system response to acute elevations of intracranial pressure (ICP), resulting in Cushing’s triad of widened pulse pressure (increasing systolic, decreasing diastolic), bradycardia, and …