How does octreotide decrease portal pressure
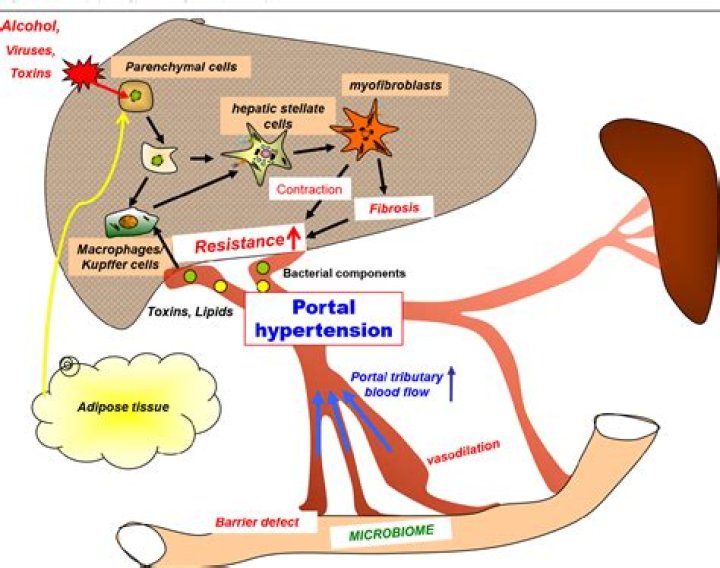
Octreotide decreased portal pressure in cirrhotic patients by inhibiting HSC contractility by decreasing intracellular Ca2+ concentration via stimulation of all SSTRs on HSCs.
How does octreotide help esophageal varices?
Octreotide reduces portal and variceal pressures as well as splanchnic and portal-systemic collateral blood flows [2]. It also prevents postprandial splanchnic hyperemia in patients with portal hypertension [3] and lowers gastric mucosal blood flow in normal and portal hypertensive stomachs [4].
How does octreotide work in cirrhosis?
Octreotide is frequently used in the ED for patients with a history of cirrhosis who present with a moderate or severe upper GI bleed presumed to be from a variceal source. Octreotide inhibits the release of glucagon, which is a splanchnic vasodilator.
How does octreotide work in variceal bleeding?
It inhibits the release of many endocrine peptides including insulin and glucagon. In addition, it inhibits the release of gastric acid. Because glucagon is a vasodilator, octreotide indirectly decreases splanchic blood flow by its action inhibiting the release of glucagon.How is portal hypertension reduced?
Medications such as propranolol and isosorbide may be prescribed to lower the pressure in the portal vein and reduce the risk of recurrent bleeding. The drug lactulose can help treat confusion and other mental changes associated with encephalopathy.
Why is vasopressin given to patients with bleeding from esophageal varices?
Vasopressin has been used for 25 years to control bleeding from esophageal varices. Its efficacy is believed to be due to a direct vasoconstrictor activity on splanchnic arterioles and precapillary sphincters, with secondary reduction in portal venous blood flow and pressure.
How do beta blockers help portal hypertension?
By slowing the heart rate and widening the blood vessels, beta-blocker medicines such as propranolol and nadolol appear to lower the blood pressure in varices that bypass the liver. In people who have esophageal varices, beta-blockers have been shown to reduce the risk of having a first episode of bleeding.
How does octreotide work in portal hypertension?
Intravenous infusions of octreotide will lower portal blood pressure and can prevent rebleeding during the patient’s initial hospitalization. Vasodilators such as isosorbide mononitrate (ISMN) reduce intrahepatic vascular resistance without decreasing the peripheral or portal-collateral resistance.Why is propranolol used for portal hypertension?
NSBBs, such as propranolol and nadolol, principally act on β1 receptors, resulting in splanchnic vasoconstriction and a reduction of portal inflow. These drugs are used for primary and secondary prevention of variceal hemorrhage.
Does Sandostatin variceal bleeding?Sandostatin injections are typically only recommended for variceal bleeding, or bleeding from enlarged veins called varices that can develop in the esophagus or other parts of the upper GI tract.
Article first time published onWhat is Octreoscan used for?
An octreotide scan (also called a somatostatin receptor scintigraphy) is a test used to check the body for neuroendocrine tumor cells. This test is done in a Nuclear Medicine department, which is a type of radiology that uses radioactive materials to diagnose or treat diseases.
How does octreotide decrease splanchnic blood flow?
Background: The vasoactive peptide octreotide has an established role in controlling variceal hemorrhage. The mechanism of action is believed to be a reduction in splanchnic blood flow. A decrease in splanchnic blood flow should be mirrored by a decrease in gastric mucosal blood flow (GMBF).
Does portal hypertension cause low blood pressure?
Hypotension is a well-known complication in patients with cirrhosis, mainly stemming from portal hypertension, which leads to splanchnic and systemic vasodilatation.
Does portal hypertension cause high blood pressure?
Portal hypertension is a leading side effect of cirrhosis. Your body carries blood to your liver through a large blood vessel called the portal vein. Cirrhosis slows your blood flow and puts stress on the portal vein. This causes high blood pressure known as portal hypertension.
Does portal hypertension increase blood pressure?
Portal hypertension is an increase in the blood pressure within a system of veins called the portal venous system. Veins coming from the stomach, intestine, spleen, and pancreas merge into the portal vein, which then branches into smaller vessels and travels through the liver.
How does vasopressin reduce portal pressure?
Vasopressin is commonly used in the treatment of bleeding esophageal varices. Its mechanism of action is thought to be splanchnic arteriolar vasoconstric- tion, resulting in a decrease in portal inflow and therefore pressure (1,2).
How do beta blockers help varices?
Beta blockers — Beta blockers, which are traditionally used to treat high blood pressure, are the most commonly recommended medication to prevent bleeding from varices. Beta blockers decrease pressure inside of the varices, which can reduce the risk of bleeding by 45 to 50 percent [1].
How does carvedilol reduce portal hypertension?
Carvedilol is a potent nonselective beta-blocker, and as such, it decreases heart rate and cardiac index (blockade of beta-1 adrenergic receptors) and causes splanchnic vasoconstriction (blockade of beta-2 adrenergic receptors), which result in a reduced portal blood flow, and thereby in decreased portal pressure.
How does vasopressin increase blood pressure?
Vasopressin selectively raises free water reabsorption in the kidneys and results in blood pressure elevation (Elliot et al, 1996).
Is vasopressin used to treat esophageal varices?
Vasopressin is widely used in treatment of hemorrhage from esophageal varices either as a systemic intravenous or superior mesenteric arterial infusion; variceal bleeding is controlled in about 50 to 60% of patients (1-8).
Why does vasopressin cause vasoconstriction?
Vasopressin is also capable of causing vasoconstriction and increasing blood pressure. … This action, which is apparently mediated by V1-receptors in the area postrema, a circumventricular organ located in the medulla oblongata, causes a leftward shift of the heart rate–arterial pressure baroreflex curve.
How does propranolol help the liver?
Propranolol hydrochloride is reported to lower portal pressure and inhibit renin secretion in patients with chronic liver disease, actions that might lessen the tendency to ascites formation.
What does portal hypertension cause?
Portal hypertension is elevated pressure in your portal venous system. The portal vein is a major vein that leads to the liver. The most common cause of portal hypertension is cirrhosis (scarring) of the liver.
Why do we use spironolactone in cirrhosis?
1 Spironolactone. Spironolactone is an aldosterone antagonist, acting mainly on the distal tubules to increase natriuresis and conserve potassium. Spironolactone is the drug of choice in the initial treatment of ascites due to cirrhosis.
What is terlipressin used for?
Terlipressin is indicated in the treatment of bleeding oesophageal varices. The administration of terlipressin serves the emergency care for acute bleeding oesophageal varices until endoscopic therapy is available.
Is vasopressin used for GI bleed?
Vasopressin is a potent vasoconstrictor which greatly reduces mesenteric blood flow. In patients with portal hypertension this results in decreased portal venous flow and portal pressure. Because of this property, vasopressin has been used for years in the therapy of variceal haemorrhage.
Is octreotide a somatostatin?
Octreotide is a medication used in the management and treatment of acromegaly and thyrotrophinomas. It is in the somatostatin analog class of drugs.
Is octreotide vasoactive?
Terlipressin, somatostatin, and octreotide are the recommended vasoactive drugs for the management of acute variceal bleeding, the comparisons between which failed to demonstrate a significant difference for the major outcomes, whereas somatostatin and octreotide were associated with better safety profiles.
How is scintigraphy done?
Scintigraphy is used to diagnose, stage, and monitor disease. A small amount of a radioactive chemical (radionuclide) is injected into a vein or swallowed. Different radionuclides travel through the blood to different organs.
What is the half life of indium 111?
Indium In 111 decays by electron capture with a physical half-life of 67.2 hours (2.8 days). The energies of the photons that are useful for detection and imaging studies are listed in Table 1.
What does elevated chromogranin A mean?
A protein found inside neuroendocrine cells, which release chromogranin A and certain hormones into the blood. Chromogranin A may be found in higher than normal amounts in patients with certain neuroendocrine tumors, small cell lung cancer, prostate cancer, and other conditions.