Can chiropractors Bill evaluation and management codes
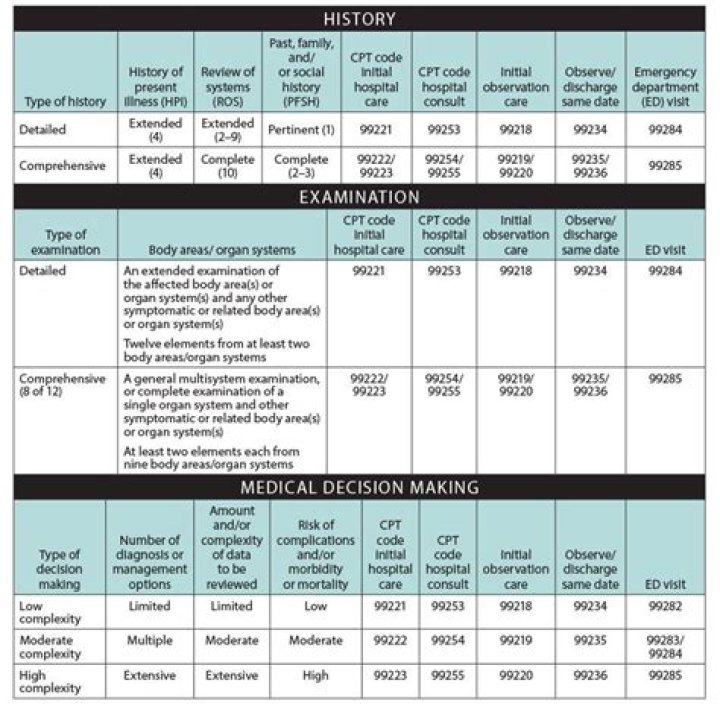
Billing evaluation and management (E&M) codes with chiropractic manipulation treatment. Billing an established office/outpatient E&M code on the same visit as chiropractic manipulative treatment (CMT) may be inappropriate since the CMT already includes a brief pre-manipulation assessment.
Can chiropractors use E&M codes?
Billing evaluation and management (E&M) codes with chiropractic manipulation treatment. Billing an established office/outpatient E&M code on the same visit as chiropractic manipulative treatment (CMT) may be inappropriate since the CMT already includes a brief pre-manipulation assessment.
Can a chiropractor bill 99213?
We have used code 99213 E&M code for office visits. However, we have some insurance companies that will cover office visits but not chiropractic treatments. … They still consider it chiropractic treatment.
What CPT codes can chiropractors bill?
- 98940 Chiropractic Manipulative Treatment (CMT) …
- 98941 Chiropractic Manipulative Treatment (CMT) …
- 98942 Chiropractic Manipulative Treatment (CMT) …
- 98943 Chiropractic Manipulative Treatment (CMT)
Can a chiropractor bill 99211?
Answer: While technically this code could be used, in reality it would be rarely used in a chiropractic office. … This code (99211) is a low complexity examination for an established patient. It can be used by chiropractors, but in most instances, it is discouraged.
Why are evaluation and management codes important?
It has been adopted by private health insurance companies as the standard guidelines for determining type and severity of patient conditions. … This allows medical service providers to document and bill for reimbursement for services provided.
Can you bill manual therapy with evaluation?
The most significant change is that 97530 (therapeutic activities) can no longer be billed with an initial PT or OT evaluation. … However, you will now be required to use a 59 modifier if you bill 97140 (manual therapy) with an initial evaluation.
How does a chiropractor bill Medicare?
This procedure, when performed by a chiropractor or other qualified provider, is covered through Medicare Part B, the component of original Medicare that includes outpatient services. Medicare will pay 80 percent of the Medicare-approved rate for this procedure. You will owe 20 percent of the amount.Can chiropractors Bill 97110?
97110 should not be billed for exercises to promote overall fitness, flexibility, endurance enhancing, aerobic conditioning, and weight reduction. However, it may be billed for maintenance of ROM or strength if the presence of a skilled therapist is needed.
What is the CPT medicine code for chiropractic treatment 4 spinal areas?CodeDescription98940CHIROPRACTIC MANIPULATIVE TREATMENT (CMT); SPINAL, 1-2 REGIONS98941CHIROPRACTIC MANIPULATIVE TREATMENT (CMT); SPINAL, 3-4 REGIONS98942CHIROPRACTIC MANIPULATIVE TREATMENT (CMT); SPINAL, 5 REGIONS
Article first time published onCan chiropractors Bill 99072?
Code 99072 may be reported during a PHE when the additional clinical staff duties as described are performed by the physician or other qualified health care professional in lieu of clinical staff.
Is manual therapy a timed code?
According to CPT guidelines, each timed code represents 15 minutes of treatment. … To give a simple example, if you performed manual therapy for 15 minutes and ultrasound for 8 minutes, you could bill two direct time units.
Can you charge an office visit with a procedure?
Can you bill an E/M service on the same day as a minor procedure? Sometimes yes, sometimes no. The decision to perform a minor procedure is included in the payment for the procedure, unless a significant and separate E/M is needed, performed and documented.
Can a chiropractor bill 99203?
While there are three primary categories of CPT codes, most chiropractors use only Category 1 codes. CPT codes in this category describe procedures performed by healthcare providers in inpatient and outpatient offices. Some examples common CPT codes used by chiropractors include: CPT Code 99203 – Initial Exam.
When should I use 99205?
99205 can be reported when the service provided requires a documented, medically necessary, comprehensive history, comprehensive exam and medical decision making of high complexity on the basis of the presenting problem for that particular date of service and the management options that are available to the physician …
Which of the following is the correct code for an extremity adjustment?
Apply 97410 Properly Per CPT® guidelines, 97140 describes manual therapy techniques, such as mobilization and manipulation, manual lymphatic drainage, and manual traction. Chiropractic adjustments have their own set of codes (98940-98942, or 98943 for an extremity).
What can be billed under therapeutic activity?
Therapeutic activities incorporate the use of multiple parameters, such as balance, strength, and range of motion, for a functional activity. Examples include lifting stations, closed kinetic chain activity, hand assembly activity, transfers (chair to bed, lying to sitting, etc), and throwing, catching, or swinging.
Can you bill manual therapy and therapeutic activity together?
Alternate Codes Alternatively, you can avoid the edit entirely by delivering interventions other than therapeutic activities (97530) when performing manual therapy (97150) during the same patient visit. … However, you cannot simply perform a therapeutic activity and bill it as a therapeutic exercise.
Does CPT code 97140 need a modifier?
The 97140 CPT code is appended with the modifier -59 or the appropriate -X modifier.
What bad effect can E&M codes have on your practice?
It is the foundation of every practice to provide quality patient care. Inaccurate medical coding can interrupt that goal, leading to frustration and confusion and a potential breakdown of the relationship you have built with valued patients.
What is the difference between E&M codes and CPT codes?
E/M stands for “evaluation and management”. E/M coding is the process by which physician-patient encounters are translated into five digit CPT codes to facilitate billing. CPT stands for “current procedural terminology.” These are the numeric codes which are submitted to insurers for payment.
Can you bill an E&M when the patient is not present?
Typically, insurers (including Medicare) will not cover an evaluation and management (E/M) service with a patient’s family or caretaker(s) if the patient is not present. … If the family member/caretaker isn’t a patient, obtain his or her demographic information so you may enter it into your practice management system.
Can a chiropractor bill 97112?
Because the description of this code includes PNF stretching, it’s often billed in chiropractic offices for muscle work performed by the doctor or a massage therapist. … For this reason, we strongly advise against using 97112 for muscle-related work within the confines of a chiropractic treatment plan.
What chiropractic CPT codes does Medicare cover?
Diagnosis Code Description Medicare Covered Chiropractic Services If the CPT code is 98940, 98941, or 98942 and is billed with one of the following primary diagnosis codes and with modifier AT, then the chiropractic service is covered.
Can you claim chiropractor on Medicare?
Medicare will pay for chiropractic care. … As part of your Medicare coverage you are entitled to up to five bulk billed chiropractic visits a year fully paid for by Medicare. This is organised by your GP through a Chronic Disease Management plan (CDM) or Team Care Arrangement (TCA).
How much does Medicare reimburse for chiropractic adjustment?
What does Medicare pay for a chiropractic adjustment? Medicare will cover 80% of the costs for these services since it falls under Part B. If you have a Medigap plan, it will cover the remaining 20%. Does Medicare require a referral to see a chiropractor?
Does 97012 need a modifier?
Whether it’s 97012 or 97140, by appending the 59 modifier, you will ensure that you receive reimbursement for both services.
What is the 8 minute rule?
The 8-minute rule is a stipulation that allows you to bill Medicare insurance carries for one full unit if the service provided is between 8 and 22 minutes.
What is the 8 minute rule in therapy?
A therapist must provide direct one-to-one therapy for at least 8 minutes to receive reimbursement for a time based treatment code. When only one service is provided in a day, you shouldn’t bill for services performed for less than 8 minutes.
What is Medicare 8 minute rule?
The key feature of the 8-Minute Rule—and the origin of its namesake—is that to receive payment from Medicare for a time-based (or constant attendance) CPT code, a therapist must provide direct treatment for at least eight minutes.
Can CPT code 96372 Be bill with an office visit?
96372 is not a separately reimbursable service when billed with an office visit.